
This needs to be worked out with your doctor. Your score should be based on what your personal best peak flow measurement would be. It’s important to talk with your doctor first before moving ahead with using a peak flow meter, ensuring your optimal score and what to do if the results drop below, are clearly documented on your written Asthma Action Plan. You will need to find your ‘best’ test score or personal best.Put in the same amount of effort (maximum) when blowing into the meter each time.Take regular readings at the same time each day rather than one-off readings.Using a chart is more useful than just written down as a list of numbers.Use this helpful log developed by the National Asthma Council Australia and Woolcock Institute for logging your lung capacity using.Reliable records will help your doctor make an accurate assessment of your asthma along with a record of asthma symptoms and reliever use, to adjust your treatment regimen. Peak flow monitoring is not recommended to be used to confirm whether you have asthma. Peak flow monitoring is not the same as spirometry and is only recommended as a guide to help you and your health professional monitor your lung function. It can also show how much your airways are changing over time if you measure your peak flow each day. This gives a general idea of how narrow your airways are. It measures the maximum (or peak) speed at which you can blow air out of your lungs. Peak flow monitoring is done with a peak flow meter. Peak flow monitoring may be an acceptable option for you after discussing with your doctor. IS THERE ANOTHER WAY TO MEASURE MY LUNG FUNCTION? To read more about lung function testing see: If a lung function test is arranged, you may notice your health professional wearing personal protective equipment.Īll services who perform lung function testing are advised to consult with their local health authority for advice on precautions around lung function testing during COVID-19. Follow this link to remind yourself of COVID-19 signs and symptoms. In case of similar symptoms, you may be asked to have a COVID-19 test and your lung function assessment postponed until your test result is confirmed negative. In settings where lung function testing is permitted and continues, it is recommended that patients are assessed for symptoms that may be similar to COVID-19. 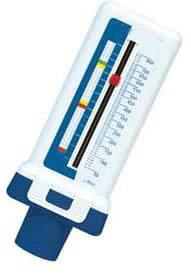
As a result, your medical practitioner or asthma treatment team may decide not to continue with lung function testing temporarily, especially if they are in a high risk area. However, it is considered a procedure that has the potential to increase the risk of respiratory virus transmission, such as that which can cause the spread of COVID-19. It is also highly recommended for asthma diagnosis. When done correctly, according to international guidelines, lung function testing can be a very useful part of your asthma management plan. Spirometry is the main recommended lung function test for the diagnosis and monitoring of asthma and other respiratory conditions like chronic obstructive pulmonary disease (COPD) in primary health care. Last updated on ACCESSING SPIROMETRY DURING COVID-19 FOR ASTHMA DIAGNOSIS OR MONITORING
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
